There are people who put off dental appointments for years, not because they don’t care, but because they dread them. Just thinking about the sounds, the smells, and the feeling of losing control puts the body on high alert. And when the body goes on high alert, the mind does the rest: it comes up with “practical” excuses to justify an emotional decision. The problem is that dental anxiety rarely stays confined to the mind. It translates into delayed pain, longer and more complex treatments, and, often, a difficult relationship with one’s own health. Conscious sedation can be a useful clinical tool in this context, but it is neither a universal solution nor a shortcut to “feeling nothing.” It makes sense when there is a clear reason, when there is a real benefit in comfort and cooperation, and when the decision is made with sound judgment and realistic expectations.
The first question isn’t “Am I afraid?”, it’s “Is fear getting in the way of treatment?”
Feeling nervous before a dental appointment is common. What makes a real difference is when that nervousness interferes with clinical care. There are some very typical signs: repeated last-minute cancellations, difficulty entering the office, trembling, sweating, nausea, shortness of breath, or a mental block that prevents the person from opening their mouth wide enough for the treatment to be performed safely. In other cases, the anxiety isn’t explosive; it’s silent. The person shows up but spends the entire appointment tense, experiences muscle pain afterward, and leaves thinking, “never again.”
Conscious sedation is appropriate when anxiety prevents treatment, when procedures are lengthy and require stability and comfort, when there is a strong gag reflex, or when past negative experiences have made cooperation difficult. The goal is not to “knock the patient out.” It is to allow the treatment to proceed with less physical stress, greater predictability, and less emotional strain.
What changes with conscious sedation and what remains the same
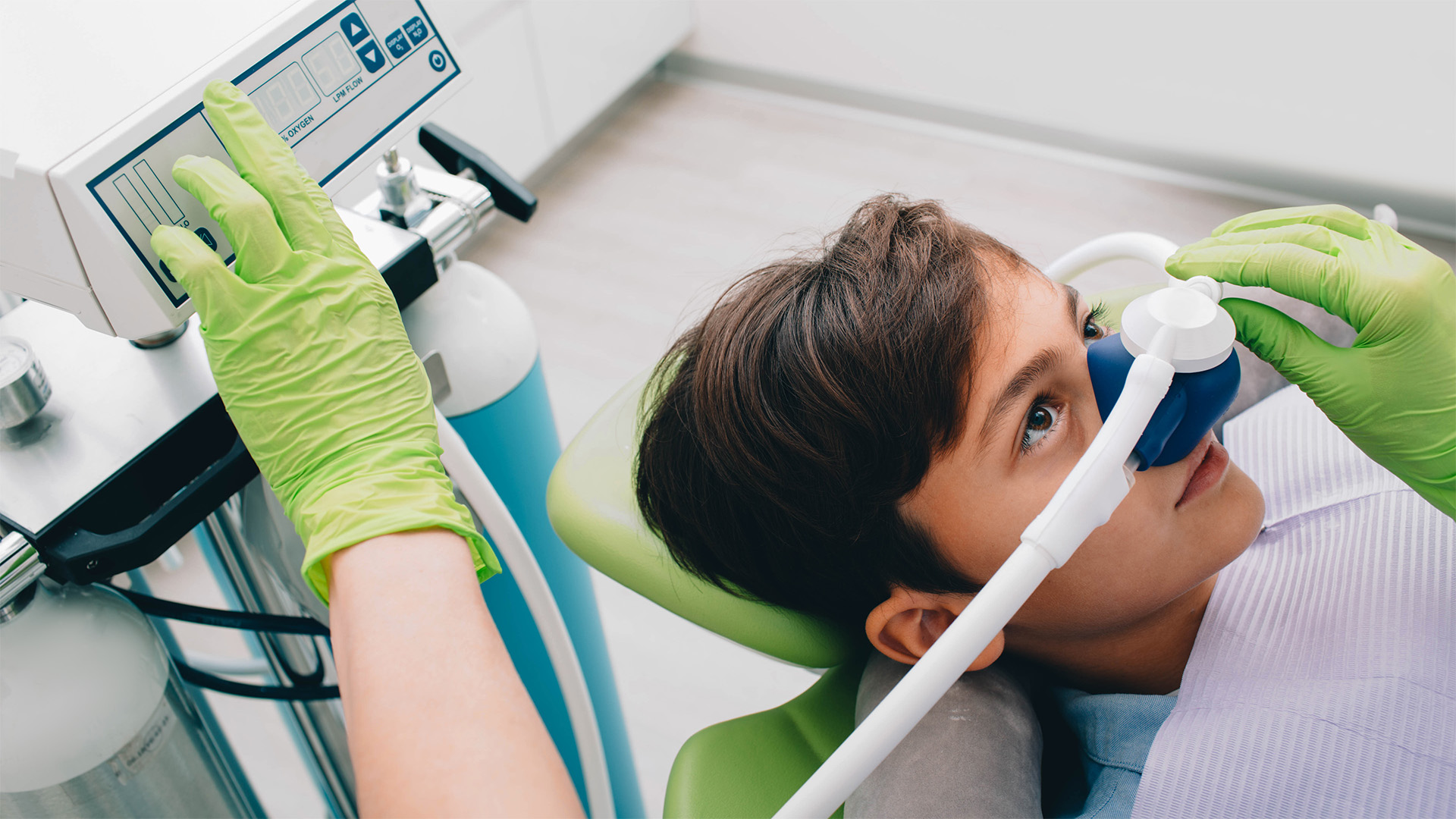
Conscious sedation is a controlled state of relaxation in which the person remains responsive and able to cooperate, but with reduced anxiety and a lower perception of discomfort. In practical terms, it changes three important things: the body is no longer in “fight-or-flight” mode, cooperation tends to be easier, and the time spent in the chair is experienced with less tension.
What remains unchanged is equally important. It is not general anesthesia. It is not “deep sleep” nor a complete loss of consciousness. Nor does it replace local anesthesia when it is necessary, because the goal is not to eliminate every single sensation. It is to reduce fear, anticipation, and reactivity, so that the procedure proceeds calmly. Those who go in expecting “I won’t remember anything and I won’t feel a thing” usually leave disappointed. Those who go in with the right expectations—less fear, more control, more comfort—tend to experience real benefits.
Who benefits the most, and who might need a different approach
Conscious sedation tends to be most beneficial for four specific groups. People with moderate to severe dental anxiety who already avoid dental care. People with a very strong gag reflex that prevents basic treatments. People who require longer procedures and, when anxious, end up being unable to tolerate the time spent in the dental chair. And people with a history of traumatic experiences in a dental setting, where the body reacts before any pain is present.
There are also situations where it is preferable to start with other strategies, or at least combine them. For mild anxiety, clinical communication techniques, shorter appointments, pacing, planned breaks, and behavioral strategies may be sufficient. Psychology is particularly useful when anxiety is part of a broader pattern, such as panic attacks, generalized anxiety, trauma, or difficulty with emotional regulation. In these cases, sedation may provide immediate relief, but addressing the underlying pattern improves the patient’s relationship with treatment in the medium term.
From a medical perspective, there are situations where the decision requires more careful evaluation, especially in people with certain respiratory or cardiovascular conditions, those using sedatives or consuming alcohol and other substances, pregnant women, or those with a history of adverse reactions. The idea is not to scare anyone. It is to treat sedation as a clinical procedure and not as an “optional extra.” If triage is done properly, safety increases and surprises decrease.
How to Make Safe Decisions: Screening, Preparation, and Monitoring
The most underestimated aspect of conscious sedation is the preparation. The decision-making process begins with the patient’s medical history, regular medications, allergies, previous experiences with anesthesia and sedation, and an assessment of anxiety levels and the type of procedure. Properly prescribed sedation is tailored to the individual. What is appropriate for one person may be excessive or insufficient for another.
Preparation includes clear guidelines on diet, regular medications, and the day’s logistics, because driving afterward is often not recommended and it may be necessary to come with a companion. During the procedure, monitoring is part of the treatment. Continuous clinical observation, monitoring of oxygenation, and assessment of vital signs are not mere details; they are what transforms “being relaxed” into “being safely relaxed.” This is also why conscious sedation must be performed by professionals with proper training and protocols, capable of recognizing any changes early on and acting appropriately.
An important point regarding realistic expectations is this: sedation is not a switch. There are varying levels and individual responses. The experience can be very peaceful, and yet the person may remember parts of the procedure. This is not a failure. It is consistent with the very concept of conscious sedation.
How do you feel afterward, and what signs should you watch out for?
After the procedure, it is common to feel mild drowsiness, some sluggishness, and a need to rest. A return to normal is usually gradual, taking several hours, depending on the method used and the individual’s profile. The recommendation to avoid making important decisions, drinking alcohol, and driving on the same day is not an exaggeration. It is basic safety.
Signs that warrant immediate medical attention are rare, but should be recognized: persistent nausea, prolonged severe dizziness, difficulty breathing, excessive drowsiness that does not improve, or any symptom that seems outside the pattern explained during the consultation. In the vast majority of cases, recovery is uneventful when there is adequate screening, correct indication, and appropriate monitoring.
The main message is that conscious sedation is not meant to “do everything at once at any cost.” It is meant to make treatment possible, comfortable, and predictable, especially for people who, without this tool, would be unable to maintain regular oral health care.
The wisest decision is the one that ensures continuity
Dental anxiety is more common than it seems, but it shouldn’t be normalized to the point of preventing people from seeking care. When a person finds a safe way to get through the appointment, the benefits extend beyond the treated tooth. It fosters continuity. It lowers the likelihood of emergency situations. It reduces the feeling of losing control. Conscious sedation makes sense when chosen based on clinical criteria, with a clear goal and realistic expectations: less fear, more cooperation, more comfort, more predictability. And that, in practice, is what allows you to schedule your next appointment without going into escape mode.
References
https://www.saad.org.uk/IACSD%202020.pdf
https://www.sdcep.org.uk/media/u23lpy1a/sdcep-conscious-sedation-in-dentistry-surveillance-review-2022.pdf
https://www.dentalcouncil.ie/wp-content/uploads/2023/06/Code-of-Practice-regarding-Sedation-in-Dentistry-May-2023.pdf
https://pubmed.ncbi.nlm.nih.gov/33711405/
https://onlinelibrary.wiley.com/doi/full/10.1111/eos.12032