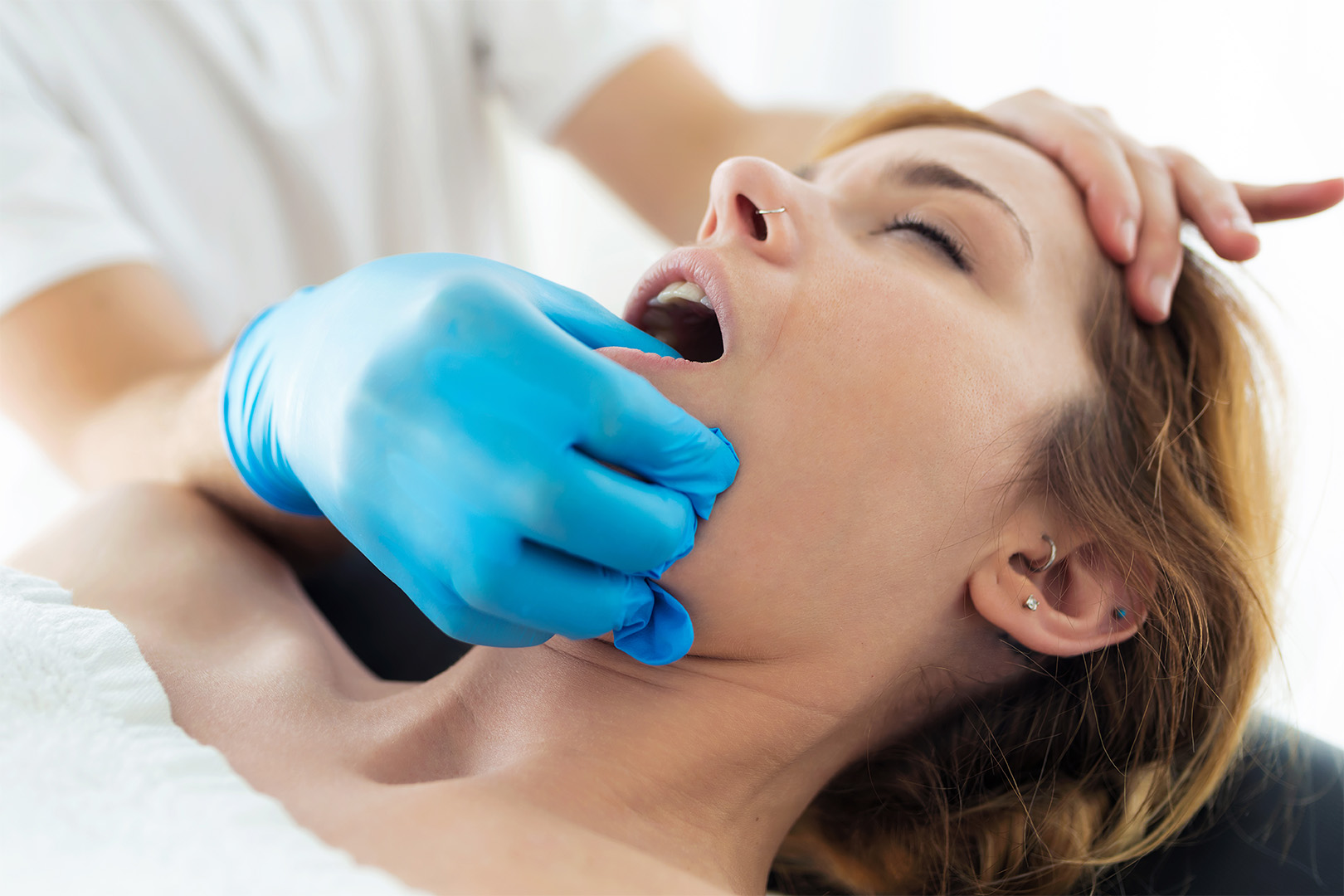
Some people only pay attention to their jaw when it starts to limit their movements. A clicking sound that comes out of nowhere, a vague pain when chewing, that “tired jaw” feeling at the end of the day, or a yawn that no longer feels comfortable. The problem is that temporomandibular disorder, or TMD, rarely comes with a clear, single warning sign. It arrives in small signs that seem like stress, poor posture, sleepless nights, or “I must have chewed wrong.” And since the discomfort comes and goes, it gets put off. Physical therapy comes into play here as a useful clinical tool precisely because it doesn’t just treat an isolated symptom. It helps restore movement, reduce pain, improve coordination, and, above all, break patterns that perpetuate the strain. The right question isn’t “does physical therapy work?” The right question is “when does it make sense, with what goals, and within what limits?”
What is DTM, and why is it not just “a snap”?
TMD is an umbrella term. It encompasses muscular, joint, and mixed disorders involving the temporomandibular joint and the masticatory muscles. Some people experience primarily muscular pain, with trigger points and muscle fatigue. Others have more joint-related symptoms, such as clicking, intermittent locking, limited opening, deviations when opening and closing, or a sensation of an unstable “snap.” There are also cases where the pain spreads to the face, temples, ear, and neck, leading to confusion with headaches, ear infections, or neck pain.
An important point is that “clicking” is not synonymous with catastrophe. There are clicks that coexist with good function. But when the click is accompanied by pain, limited range of motion, fatigue, or locking, it ceases to be a minor detail and becomes a sign that the mechanics are unstable. The clinical diagnostic tools most commonly used in research and practice, such as DC/TMD, reinforce exactly this logic: distinguishing what is predominantly muscular from what is predominantly joint-related, because the treatment approach may change.
When is physical therapy appropriate, and what are the expected outcomes?
Physical therapy is recommended when there is pain associated with chewing, limited mouth opening, muscle fatigue, clicking sounds accompanied by discomfort, a feeling of stiffness upon waking, pain that worsens with prolonged talking, or when patterns of neck tension and poor posture appear to be contributing to jaw symptoms. It also makes sense when the person is unconsciously “clenching,” or when there is suspicion of sleep bruxism or daytime clenching exacerbating muscle overload.
The goals need to be concrete. Reduce pain, increase opening range without fear, improve jaw coordination, reduce bodily hypervigilance, and restore confidence to eat and speak without avoiding certain movements. In many cases, the goal is not to “never feel anything again.” The goal is to regain a predictable jaw. The person stops thinking about their jaw at every meal. This is a relevant clinical indicator, because chronic pain intensifies when the body enters a cycle of protection and anticipation.
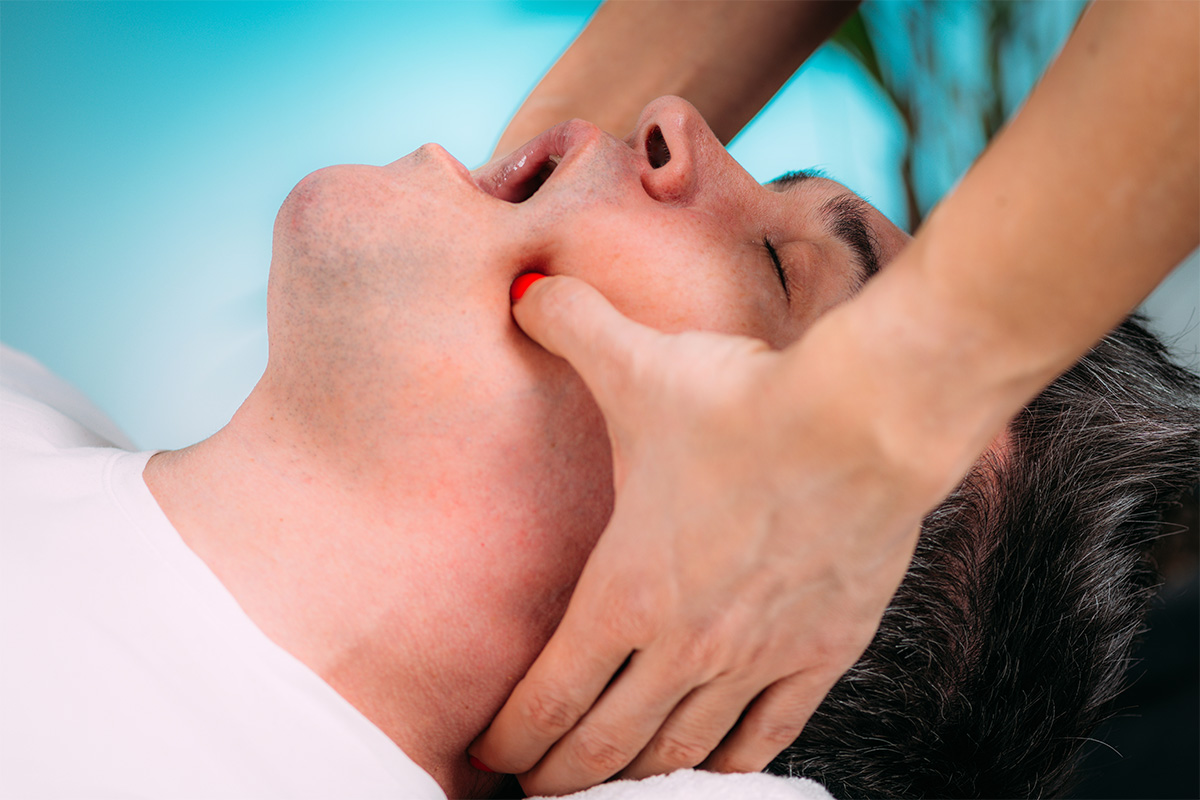
What physical therapy actually does, in practice, without making empty promises
Physical therapy for TMD is typically multimodal. In simple terms, it combines education, training, and manual intervention, depending on the case. Education involves explaining what aggravates symptoms and how to reduce daily stress without living under constant restriction. Training includes exercises for motor control, coordination, and, in some cases, strengthening and selective relaxation. Manual intervention may include techniques targeting the masticatory and cervical muscles, as well as gentle mobilizations when the joint is stiff or when a protective pattern is present.
Recent evidence from systematic reviews suggests that physical therapy approaches, especially when they include exercises and self-care components, can reduce pain and improve function in TMD, although the response varies depending on the type of TMD and the quality of the protocols. Specific reviews on exercise therapy point to benefits, particularly for painful TMD. There are also classic clinical trials showing additional gains when structured exercises are added to self-care for myofascial pain.
The value of this evidence lies not in turning physical therapy into a miracle cure, but in confirming that, for many patients, addressing motor control, load, and the system’s sensitivity has a real impact—especially when treatment is consistent and the plan is tailored to the specific subtype of TMD. And here lies an important limitation: there is no single exercise that works for everyone. What works in a case of myofascial pain may be insufficient in a case of joint blockages, and vice versa.
What might be hindering progress, and when is it necessary to coordinate with other approaches?
There are three common triggers. The first is continuing to “strain” the joint without realizing it. Clenching your teeth when concentrating, always chewing on one side, biting your nails, chewing gum all day, resting your chin on your hand, forcing yourself to yawn, or insisting on eating very hard foods when the pain is active. None of these habits is a sin. They are automatic patterns. But they fuel TMD.
The second obstacle is stress and sleep. Not because “TMJ is psychological,” but because the nervous system in alert mode increases muscle tension, lowers pain thresholds, and hinders recovery. If a person sleeps poorly, their ability to self-regulate during the day decreases and clenching tends to increase. In some cases, addressing sleep and anxiety in parallel accelerates results—not by magic, but by reducing the overall burden on the system.
The third obstacle is an incomplete diagnosis. There are situations in which physical therapy is helpful but is not sufficient on its own. Teeth with problematic occlusal contacts, the need for a mouthguard in selected cases, neuropathic pain, inflammatory arthritis, trauma, or suspected specific disc dislocations may require coordination with dentistry, general medicine, or, when indicated, other specialties. A responsible clinical approach is conservative and reversible as a first-line treatment, but it is not blind. If there are signs of persistent locking, severe limitation, progressive pain, marked loss of function, fever, swelling, or neurological symptoms, this calls for a more in-depth evaluation.
How to make a confident decision and what’s worth keeping
Physical therapy is effective for TMD when the goal is to restore function, reduce pain, and break the tension-protection-limitation cycle. It is most effective when there is a clear diagnosis of the TMD subtype and when the treatment plan is tailored to the individual case, with realistic expectations and ongoing follow-up. Most people don’t need to live with their jaw “on high alert.” They need a plan that addresses what lies behind the symptom, not just the symptom itself.
The most valuable outcome is usually simple: being able to chew, yawn, and speak again without thinking about it. When that happens, TMD stops taking up mental space. And that is one of the best signs that the system has regained predictability. At Clinicalvor, physical therapy for temporomandibular disorders can be an important step when your jaw starts to limit your daily life, especially when the discomfort is no longer occasional and when your body is sending signals that shouldn’t be ignored.
References
https://pubmed.ncbi.nlm.nih.gov/24482784/
https://pmc.ncbi.nlm.nih.gov/articles/PMC10299279/
https://pmc.ncbi.nlm.nih.gov/articles/PMC10382173/
https://academic.oup.com/ptj/article/86/5/710/2857458
https://www.jofph.com/articles/10.11607/jofph.21.4.06
https://wexnermedical.osu.edu/-/media/files/wexnermedical/patient-care/healthcare-services/sports-medicine/education/medical-professionals/other/temporomandibular-joint-disorder.pdf