Dental prosthesis can restore confident chewing, more natural speech, and a smile that doesn’t need “disguises.” Still, it’s normal for the adjustment not to happen overnight. The mouth is living tissue, with sensitivity, saliva, pressure points, and a very concrete neuromuscular memory. When the way teeth touch and how force is distributed changes, the body needs to recalibrate. What creates frustration is not the prosthesis itself, but the expectation that everything will feel natural right away. This article explains, with clinical clarity and without drama, what influences comfort and aesthetics, what tends to be normal in the first few weeks, and when it makes sense to reassess, in line with the logic of rehabilitation and follow-up provided by the Dental Prosthetics department.
What is a dental prosthesis, and why is there no “one-size-fits-all” solution?
The term “denture” is often used as if it were a one-size-fits-all solution, but in practice, it is not. There are removable dentures, fixed dentures, and implant-supported dentures, and each type relies on a different mechanism of support and retention. This changes almost everything: the feel in the mouth, stability, hygiene, and the adjustment period. A removable prosthesis rests on the mucosa, and when there are remaining teeth, it may have components that aid in retention. A fixed prosthesis tends to provide a greater sense of stability because it relies on rigid supports. An implant-supported prosthesis no longer depends solely on the compressibility of the tissues and can improve retention in specific cases, especially when achieving stability with a removable prosthesis is difficult. This is why it makes no sense to compare “my denture” with “my family member’s” as if they were the same treatment. They are often different solutions, in different mouths, with different clinical histories.
Adaptation is also learning: the mouth and the brain have to work together
Even when there is no pain, it is common to feel some initial discomfort. The prosthesis alters internal volumes and changes the usual path of the tongue and cheeks during speech and chewing. The brain has to reorganize automatic patterns. That is why subtle changes in diction, fatigue when chewing, and a sensation of “having something there” may occur for a while. This tends to be more evident with extensive removable dentures, especially full dentures, because there is a base in contact with the mucosa and a new interaction with saliva.
What matters clinically is the trajectory. If there is gradual improvement from week to week—even if slow—the process is proceeding as expected. If there is discomfort that recurs in the same spot without any improvement, this indicates a need for adjustment. Expectations also play a role. Those who expect “immediate perfection” interpret every sensation as a failure. Those who enter with a realistic goal—progressive comfort through fine-tuning—tend to adapt better and continue with the treatment.
What determines everyday comfort: stability, bite, saliva, and support
Comfort depends, above all, on stability. A denture that shifts when speaking, tilts when chewing, or creates pressure points causes anxiety and irritates the oral mucosa. Stability is also emotional: when a person feels confident that the denture won’t move, they eat better, speak more naturally, and smile more freely.
Bite alignment is another decisive factor. Minor “high” contacts can concentrate force at a single point and cause localized pain, a feeling of instability, or muscle tension. Even without getting into unnecessary technical details, the logic is simple: well-distributed forces tend to provide greater comfort. Saliva quietly enters the equation. In a dry mouth, the mucosa becomes more vulnerable to friction and retention worsens, especially with removable dentures. Xerostomia caused by medication, age, mouth breathing, or other factors can make adaptation more challenging, even with a well-made denture.
Bone support and anatomy also play a role. In cases of marked bone resorption, especially in the mandible, the “foundation” is smaller and the stability of a removable prosthesis can be more difficult to achieve, even with a good design. In such cases, it may make sense to discuss alternatives that increase retention, including implant-supported solutions when clinically indicated, because there are biomechanical limitations that cannot be overcome by sheer willpower.
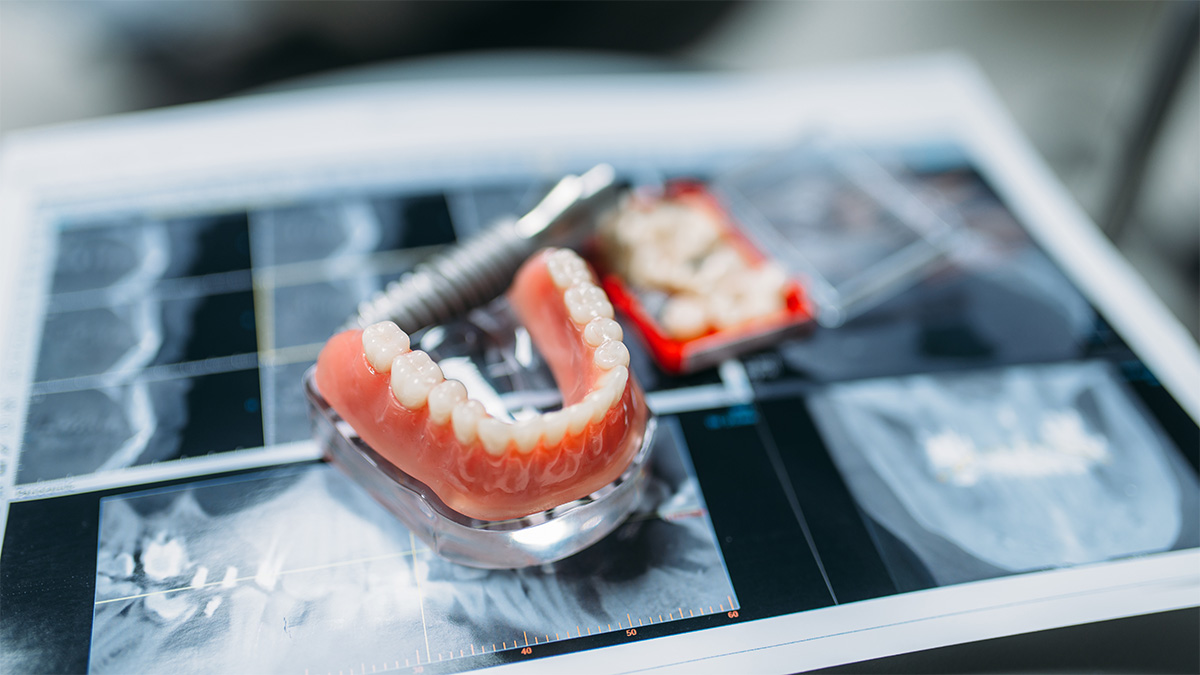
The First Few Weeks: what’s normal and what often causes problems
In the first few weeks, it is common to experience sensitivity at specific points, especially with removable dentures. There may also be a period of adjustment when it comes to speech, as well as some fatigue when chewing thicker foods. The typical course of recovery involves gradual improvement, provided that pressure points are addressed and the person does not try to compensate by using “workarounds.”
Adjustments made during follow-up visits are part of the process and should not be viewed as a failure. A denture may be generally well-fitting yet still require minor adjustments to eliminate areas that irritate the mucosa. What often causes problems is forcing the denture despite significant pain, attempting to adjust the denture without professional guidance, or using adhesives as a permanent solution to stability issues instead of addressing the underlying cause.
Hygiene is another non-negotiable factor, because dentures accumulate biofilm. When biofilm is present, inflammation occurs and the risk of denture stomatitis increases, especially if the dentures are worn for many hours at a time without giving the tissues a break. The oral mucosa needs time to recover. Adaptation improves when there is a proper cleaning routine and when the denture is maintained, not just “put in and forgotten.”
When to reassess: signs you shouldn’t ignore
Some initial discomfort is to be expected, but certain signs warrant a reevaluation. Pain that does not improve after adjustments, recurring sores always in the same spot, persistent instability that prevents safe speaking or chewing, burning and marked redness of the mucosa under the denture, or a sensation of an “uneven” bite that causes muscle tension are all reasons to seek a consultation. Any sudden change in a denture that was previously well-fitted also warrants evaluation, as it may indicate wear, fracture, changes in the supporting base, occlusal changes, or progression of an oral condition.
A common mistake is getting used to eating less well, speaking with less confidence, and accepting discomfort as “normal.” A prosthesis should allow for a normal life. If it doesn’t, something needs to be adjusted, reviewed, or, in some cases, rethought to find the most appropriate solution for that situation.
What changes when there is support and well-aligned expectations
Adaptation isn’t always immediate because it involves stability, bite, oral mucosa, saliva, and neuromuscular relearning. When the treatment plan is well-suited to the case, the work is done with care, and there is follow-up with adjustments and maintenance, the trend is toward progressive improvement and real comfort in daily life. The goal is not for the person to simply “put up with” it. It is for them to feel confident chewing, at ease speaking, and comfortable living. A well-managed prosthesis ceases to be an object that is merely tolerated and becomes a functional solution that integrates seamlessly. The difference between giving up and adapting often lies in small corrections made at the right time and in realistic expectations, without quick promises or improvisation.