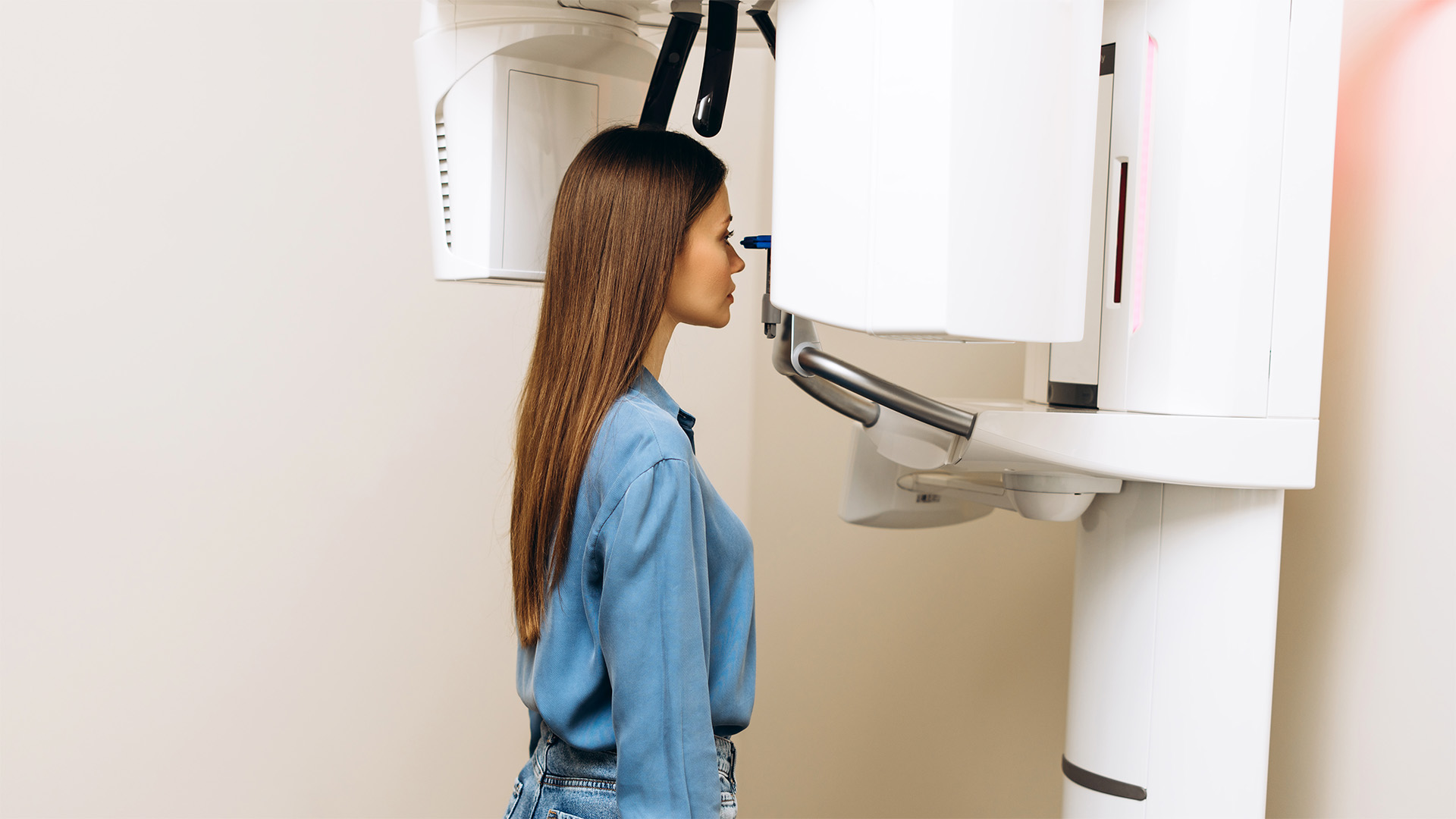
There are consultations where the problem is plain to see: an obvious fracture, a painful cavity, or inflamed gums. And there are others where the pain is present, but the surface doesn’t explain it. That’s when radiology ceases to be “just a test” and becomes an integral part of the diagnosis. Seeing clearly isn’t about curiosity; it’s about avoiding decisions based on assumptions. At Clinicalvor, radiology incorporates advanced technology for precise diagnoses, including CBCT and orthopantomography, and is used for both diagnosis and treatment planning, especially when the details change the treatment plan and ensure patient safety.
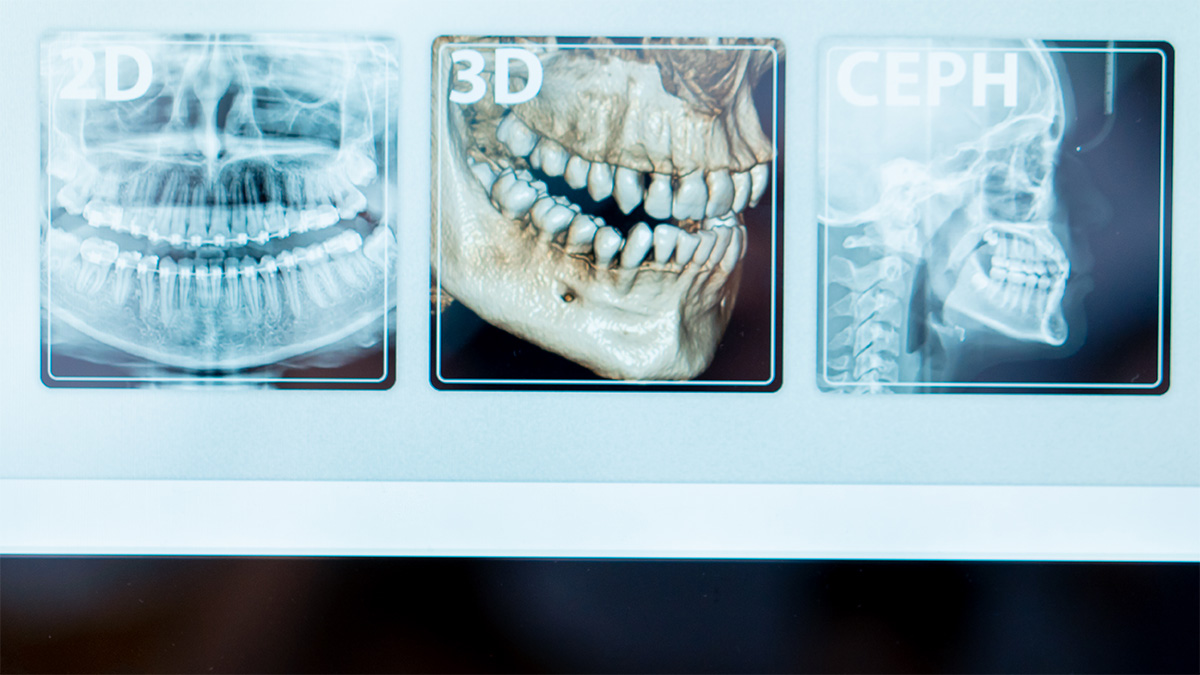
What is 3D dental radiology, and how does it differ from 2D?
A 2D X-ray shows a two-dimensional image. It is useful, quick, and, in many cases, sufficient. The problem is that the mouth is not flat. Roots, nerves, bone, maxillary sinuses, and impacted teeth exist in three dimensions, and 2D imaging can overlap structures and obscure relevant details. 3D radiology, typically via CBCT, creates a volumetric image that allows for much more precise assessment of bone thickness, anatomical relationships, and pathways. This does not mean it is “better” by definition. It means it answers questions that 2D cannot answer with the same reliability.
The orthopantomogram, on the other hand, is a 2D panoramic scan that provides an overview of the teeth and jaws. It is often the first comprehensive image, useful for triage and initial planning. When the panoramic scan raises a question that could alter the clinical decision, 3D imaging comes into play as a precision tool.
For those to whom it applies: cases where the details actually change the plan
Not everyone needs a CBCT. The golden rule is justification. It makes sense when the additional information changes the treatment plan or reduces risk. In implantology, for example, 3D imaging can be crucial for assessing bone volume, the proximity of anatomical structures, and planning implant placement more safely. In cases of impacted wisdom teeth, especially lower ones, it can be important to understand the relationship with the inferior alveolar nerve and anticipate risk, helping to choose the most prudent surgical approach.
In endodontics, 3D imaging can be useful in complex anatomies, retreatments, suspected root fractures, resorption, or when symptoms do not match what 2D imaging shows. In orthodontics and oral surgery, it can assist with impacted teeth, significant asymmetries, and situations where the actual position of a tooth or root determines the treatment strategy.
There are also contexts involving dental trauma, fracture assessment, and oral rehabilitation planning where a three-dimensional view reduces uncertainty. The idea is not to replace the clinical examination. It is to provide context.
Safety and radiation: what you need to know without overreacting
The topic of radiation gives rise to two common misconceptions. The first is outright fear, as if any X-ray were dangerous. The second is to downplay it, as if it were an irrelevant detail. The balanced clinical approach lies somewhere in between: use it when it makes sense, with the smallest field of view and lowest dose necessary to answer the clinical question.
The European guidelines for CBCT in dento-maxillofacial radiology reinforce precisely this. Justify each exam, optimize the protocol, and prefer smaller fields of view whenever possible. The effective dose of a CBCT varies greatly between devices and protocols and can differ by more than tenfold, especially depending on the field of view and exposure settings. There are classic studies that quantify this variation and show that there is no universal “one dose” for CBCT. That is why the correct clinical discussion is not “CBCT is too much” or “CBCT is too little.” It is “do I really need 3D to make a confident decision?” and, if so, “what is the minimum field of view for my case?”
In practice, this translates into a responsible medical decision: the diagnostic benefit must outweigh the radiological cost, and the examination must be performed using parameters tailored to the objective.
What a medical exam aims to achieve: diagnosis, planning, and avoiding surprises
Clinicalvor’s radiology page describes these exams as quick and non-invasive, useful for seeing beyond the surface and identifying problems that might otherwise go unnoticed, thereby supporting diagnosis and treatment planning. When translated into clinical practice, this concept has a simple consequence: fewer surprises during treatment.
In dentistry, “surprise” usually means extra time, additional procedures, more discomfort, and, at times, decisions made on the spot. Planning supported by appropriate imaging reduces this likelihood. In oral surgery, it helps anticipate difficulties and anatomical risks. In implantology, it helps determine positioning and the need for complementary approaches. In endodontics, it helps determine whether there is a structural cause for persistent pain.
It is also important to emphasize that radiology is not just for “finding the problem.” It serves to avoid unnecessary treatments. When the image shows that the most feared hypothesis is not confirmed, that is equally valuable.
What to expect on exam day and what tends to scare people for no reason
For most people, the exam is simpler than they imagine. It doesn’t hurt, doesn’t require any complicated preparation, and takes very little time. Anxiety usually stems from two sources. The first is the word “CT scan,” which brings to mind lengthy hospital exams. The second is the idea that radiation is inevitably dangerous.
The most helpful approach is to frame it clearly: the purpose of the exam is to guide a clinical decision with greater precision. If the dentist orders it, it’s because there’s a question that 2D imaging can’t answer with the necessary certainty. And when the exam is properly indicated, the benefit is reduced risk and increased predictability.
After the exam, clinical interpretation is the crucial step. A 3D image is not a diagnosis in and of itself. It is information. The difference lies in who interprets it, how they integrate it with the clinical exam, and how they translate that into a treatment plan.
What to keep in mind before making a reservation
3D radiology isn’t for everyone, and it isn’t just for “seeing better for the sake of it.” It’s for cases where detail changes the decision, improves planning, and reduces risk. The orthopantomograph provides a useful and quick overview. CBCT comes into play when it is necessary to understand depths, anatomical relationships, and structures that 2D imaging may obscure. The correct decision is always the simplest one that answers the clinical question. When the exam is justified and optimized, the patient gains something very concrete: clarity. And clarity, in dentistry, usually saves time, discomfort, and surprises.
References
https://www.clinicalvor.pt/medicina-dentaria/radiologia/
https://op.europa.eu/en/publication-detail/-/publication/ec5936c7-5a29-4a93-9b3a-01a5d78d7b2e
https://www.sciencedirect.com/science/article/abs/pii/S0720048X10005826
https://pmc.ncbi.nlm.nih.gov/articles/PMC4277388/
https://www.physicamedica.com/article/S1120-1797%2821%2900251-9/abstract